The Antimicrobial Resistance Channel – uniting the four pillars of AMR research
PLOS, in collaboration with the Global Antibiotic Research and Development Partnership (GARDP), is delighted to launch the Antimicrobial Resistance (AMR) Channel. This new Channel offers the AMR research community access to the latest research, as well as commentaries, blogs, news and discussions that span science, research and development, public health, and policy in the fight against AMR.
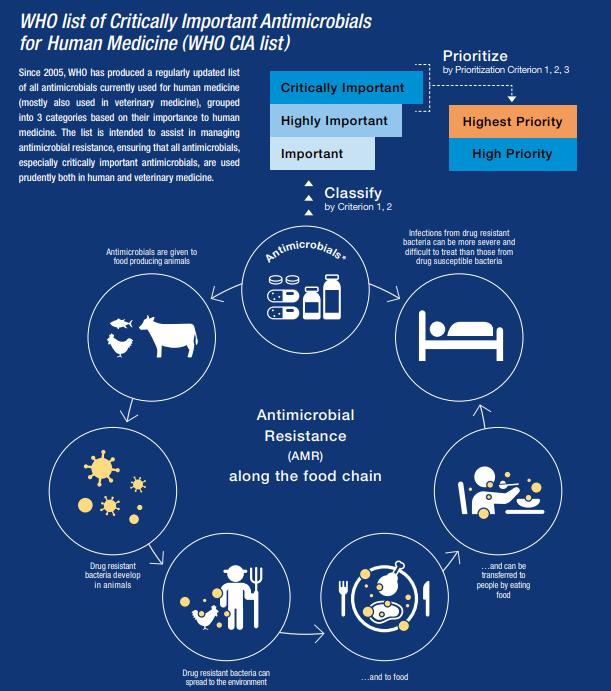
Antimicrobial Resistance is a serious threat to global public health that requires action across all sectors and society. Despite the international attention directed at AMR, and many policy discussions for developing new antibiotics accessible to all, the situation remains a major global concern. Key challenges include improving infection prevention, limiting unnecessary use of antibiotics, and using existing antibiotics appropriately in humans, animals, and in agriculture.
The PLOS AMR Channel is a resource for the AMR community to discover, explore and keep up to date with the latest scientific literature, commentaries, blogs, and news. Channel Editors comprise leading experts who will collate content to increase awareness of the AMR crisis, encourage research collaboration that integrates science, policy and public health, as well as highlight critical content in the fight against AMR. A holistic approach to research is urgently needed to provide the evidence-base for well-informed policy-making, governance, and funding.
Siloed research will not be effective in addressing AMR. The PLOS AMR Channel will highlight four pillars of AMR research (Basic Science – biology of disease, Research and Development, Appropriate Use and Access, Public Health – surveillance and epidemiology), but the Channel Editors are united in the belief that a coordinated, integrated, and prioritised research agenda is required to effectively ensure these areas form a singular public health response. The AMR Channel provides a space where these fields are brought together in one platform, and challenges researchers to think beyond individual research domains.
“Developing new treatments to tackle AMR is an important global priority. However, doing so in isolation of stewardship, access and surveillance jeopardizes the public health return on investment of developing accessible treatments,’ says Dr Manica Balasegaram, Director of GARDP and one of the Channel Editors. He continues ‘It’s important to move away from working in silos and find ways of bringing together the latest science, policy and public health research if we are to successfully address the challenges in AMR.”
The Four Pillars of Antimicrobial Resistance
Basic science – the biology of disease
Advances in the basic scientific understanding of microbes and host responses that are relevant to the discovery of new treatments including antibiotics are key to the battle against AMR. Finding new microbial targets that are druggable, emphasizing the interface between chemistry and biology, is especially important.
Channel Editor: Patricia Bradford
Deputy Channel Editor: Laura Piddock
Research and Development (R&D)
R&D into new treatments and health tools is not happening fast enough. Incentives to develop new antibiotics are slowly being introduced, but the deliverables are often poorly aligned with clinical needs. New diagnostic tools are needed to quickly and accurately identify the cause of infection and/or whether antibiotics are required. Ideally, these should be usable in areas with poor access to electricity and laboratory expertise. Such tools will help optimise treatment and reduce wasteful empirical use.
Channel Editor: Manica Balasegaram
Deputy Channel Editor: Ursula Theuretzbacher
Appropriate use and Access
Overuse and misuse of antibiotics in humans and in animals coupled with poor infection control are the main drivers for the development and spread of AMR. Antimicrobial stewardship, originally applied as initiatives in hospitals to promote more appropriate antibiotic use, has now become a term for actions in all levels of society that promote responsible antibiotic use. There is a great need for globally agreed ‘rules of the game’ to set the stage for both responsible use of existing antibiotics and for the introduction of new ones. This also includes a better understanding on when and how use of antibiotics in animals affects resistance in microbes that cause infections in humans, and how this can be managed.
Channel Editor: Peter Beyer
Deputy Channel Editor: Ingrid Smith
Public health – Surveillance and epidemiology
Decision-making in effectively addressing AMR is driven by timely and accurate information. Gathering data on the emergence and spread of antibiotic resistance is important. However, simply monitoring or surveilling AMR without implementing interventions to reduce AMR will not be helpful in the long run. Surveillance, although incomplete for some countries, has already revealed that antimicrobial resistance is a global threat affecting rich and poor countries. Surveillance outcomes can be used in a rationale for changes in societal investment; for instance to determine whether specific treatments are productive when measured against improvements in QALYs (quality-adjusted life years). This is also where public health needs and priorities must inform R&D of health tools.
Channel Editor: Iruka Okeke
Deputy Channel Editor: Carmem Pessoa-Silva
The four pillars of AMR research require concerted and integrated action. Working in silos will be ineffective if we are to maintain life-saving antimicrobial medicines. Global approaches across all sectors are required. The goal of the PLOS AMR Channel is to break down these silos and facilitate collaboration and coordination to respond to this global health threat.
Check out the PLOS Antimicrobial Resistance Channel: channels.plos.org/amr

Great Initiative !
But why you did not make another pillar about Medicines quality. Poor quality medicines is major contributing factor to microbial resistance in general and not only resistance to antibiotic.
I very much agree that we must have co-ordinated, integrated and prioritised research into AMR. The topic is now beginning to be taken seriously and funding is being made available. There are many questions and issues to be addressed. Taking the 4 pillar construct, we have to be careful that funders do not all fund one pillar or even the same bricks in a particular pillar. This would reduce the speed of a successful resolution to this global problem. As funders we need to get together and ensure that we fund research across the field. It is very easy for us all to want to fund the “sexy” topics. A road map of who is funding what would be very useful We also need to make sure that we exploit the outputs from research. We are all conscious of “valleys of death” along R&D pathways. Clear road maps may mitigate this to some degree.
One of my bug-bears is how as a community can we recognise good ideas as they are being delivered, and how can we continue funding them without the need to wait for a relevant call to open and a long application process to be completed. Perhaps I am being too much of an idealist!
Innovate UK currently have a call out in conjunction with China (MoST). My hope is that any useful outputs that come out of this are picked up and further developed without ant delay.
Please see a link to a recent blog.
http://ow.ly/YJtB30jNfNi
Siloed research has not only delayed progress in addressing AMR, but has hindered consensus among stakeholders on what constitutes a comprehensive approach to this global threat. The Antimicrobial Resistance Channel’s third pillar, Appropriate Use and Access, should more clearly encompass the need to ensure antimicrobial quality, especially because treatment failure as a result of poor-quality medicines may be assumed to be due to a resistant infection. AMR program planners generally do not include a consideration of medicine quality; even though exposure to sub-therapeutic doses due to substandard or falsified medicines may mimic conditions that were reported to promote bacterial resistance. This risk is greatest in low- and middle-income countries, where WHO has estimated that 10% of all medical products are substandard or falsified. The Promoting the Quality of Medicines (PQM) program, funded by the U.S. Agency for International Development and implemented by the U.S. Pharmacopeia, recommends that the Antimicrobial Resistance Channel expand its third pillar to include these critical concepts and suggests renaming the pillar as “Appropriate Use and Access to Quality-Assured Medicines.” We look forward to the potential collaboration and engagement that this new channel can bring to the fight against AMR.