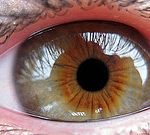
Treating Trichiasis
Guest blogger Dr Michael Ekuoba Gyasi discusses trachoma, and the implications of two trials recently published in PLoS Medicine evaluating the treatment of minor trichiasis.
Trachoma is caused by Chlamydia trachomatis and is a leading cause of infectious blindness. In endemic communities the disease normally runs a chronic course with two distinct stages. The active stage occurs mainly in children under ten years who experience inflammation of the eyelids and discharge from the eye. The second stage occurs mostly in female adults. This is believed to be due to their close association with children, who serve as the reservoir for C. trachomatis, leading to cycles of re-infection and healing. With the ensuing chronic inflammation of the tarsal conjunctival tissues the lid margins turn inwards (entropion) and the lashes eventually touch and rub the surface of the globe (trichiasis) leading to corneal opacification and visual impairment.
Trachoma has been eliminated in most parts of the developed world but the disease remains a major cause of avoidable blindness in many developing countries. At the global level the disease is concentrated in hot, dusty, and dry parts of the world stretching from Africa, through the Middle East to the Indian sub-continent and Asia with some pockets in Latin America. In endemic countries, it is found in rural areas that are economically underdeveloped with limited access to water and generally low level of personal and environmental hygiene.
As an infectious disease, trachoma clusters at the household and community levels with different severity and different potential for blindness. Ocular discharges containing the Chlamydia organism are the main sources of infection, which is transmitted through fomites (any inanimate object capable of carrying an infection), contaminated fingers and, more importantly, the eye-seeking common housefly, muscae sorbens.
The World Health Organization currently estimates that Trachoma accounts for 3.6% of global blindness burden and a control program, the SAFE strategy is being implemented in affected countries under the tenets of Vision 2020, the Right to Sight initiative. While there has been considerable success in the control of active trachoma in many endemic countries, the same cannot be said of the vision-threatening inactive form of the disease. The many reasons for this include inadequate number of surgeons trained to perform lid-rotation surgery, high recurrence of operated cases, low acceptance of corrective surgical procedures and socio-cultural issues among others. It is in this light that any attempts aimed at increasing surgical uptake, improving success and exploring alternative solutions should be commended.
A recently published high-powered control study by Rajak and co-workers has shown that using absorbable sutures (polyglactin-910) for tracomatous entropion surgery is as good as using conventional non-absorbable silk sutures. Using the same surgical techniques, the authors found no difference in recurrence rate between the two sutures, even though there have been previous reports favouring lower recurrences for polyglactin. Since polyglactin sutures are absorbable and thus can be left in-situ, they offer major advantages in the operational sense; removing sutures is less of a burden for patient and surgeon freeing time to move on with other surgeries. It also allows surgeons enough time to assess surgical outcome and potential for recurrence. The main drawback however, is the cost and availability of polyglactin sutures in many of these impoverished countries where trachoma is endemic. Control programs will have to make budget allocation for this or persuade the manufacturer (Ethicon) to make donations in the same way as Pfizer and others do for azithromycin.
While surgical management of entropion is the gold standard for preventing cornea opacification and visual impairment, high recurrence rate, limited access, economic and socio-cultural barriers prevent many trachoma patients from accepting surgery in all cases. An alternative approach that is effective, easy to deliver and culturally acceptable therefore becomes important. This is why a sister article by Rajak and colleagues looking into the inferiority of self-epilation to standard surgical management of mild trichiasis is worth reading. Though inconclusive, there is enough evidence that self-epilation could be a viable alternate approach to the prevention of trachomatous corneal blindness.
Dr. Michael Ekuoba Gyasi is Medical Director of the North Western Eye Centre and Head of Clinical Care and Research at the Emmanuel Eye Centre in Accra, Ghana.