The fight for a malaria-free Bangladesh
On World Malaria Day, Kasturi Haldar, Editor-in-Chief of PLOS Pathogens, Bernard Nahlen and Neil Lobo from the University of Notre Dame and Mohammad Shafiul Alam and Wasif Ali Khan from the International Center of Diarrheal Diseases, Bangladesh (icddr, b), comment on advances in malaria control and elimination in Bangladesh, which lies on a historical path of the global spread of drug resistant malaria.
From 2010 to 2018 Bangladesh achieved remarkable success and reduced malaria cases by 81% http://www.nmcp.gov.bd/. However, 2019 showed increase in malaria cases. Over 90% occur in the Chittagong Hill Tracts (CHT) districts (Khagrachhari, Rangamati and Bandarban) where hundreds of thousands of refugees have fled to from Myanmar, increasing the threat of spread of drug resistant parasites.
The elimination of malaria is defined at achieving three consecutive years of zero locally-acquired malaria. Bangladesh’s National Strategic Plan (2017-2021) has set a target for a malaria-free Bangladesh by 2030. Led by the National Malaria Elimination Program (NMEP) and in partnership with BRAC (the world’s largest NGO, indigenous to the country), Bangladesh plans phased elimination, targeting (i) eight northeastern states by 2021 (ii) the Chittagong region including Cox’s Bazar presently the world’s largest refugee settlement, by 2025 (iii) the three ‘endemic’ CHT districts, by 2030 (National Strategic Plan for Malaria Elimination: 2017-2021, Dhaka Bangladesh 2017), all the while preventing re-introduction in areas free of malaria and the emergence of resistance to artemisinin-based combination therapies, front-line antimalarials key to malaria control. Regrettably artemisinin resistance has emerged in Myanmar and other countries in the Mekong region.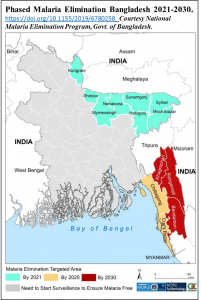
From 2017 onwards, Bangladesh has mobilized significant financial and human resources from national and international sources such as the Global Fund to strengthen health systems, improve malaria surveillance and response capability, and invest in advanced research to address the growing threat of drug and insecticide resistance. 60% of malaria occurs in the Bandarban district in the CHT. It is therefore critically important to develop research and implementation capacity in high transmission areas like Bandarban to ensure that evidence-based control measures continually support the national elimination program.
In addition, transmission of vector borne diseases such as malaria are directly affected by changes in rainfall, temperature and humidity, so attention to climate factors is also key to interpreting trends in malaria cases and deaths. Bandarban showed marked increase in rainfall late in 2019 (as well as some increase late 2018). Increasing rainfall in conjunction with recent data showing emergence and spread of insecticide resistance in the Bandarban region (Alam M.S. et al.2020 Am. J. Trop. Med. Hyg; accepted for publication) points to the need for more research to combat these gaps in protection.
Bangladesh’s innovation in revival of its economic engine and delivery of effective, low-cost healthcare will be needed to position the country to address immediate challenges posed by COVID-19 and other future disease threats. On World Malaria Day, we celebrate Bangladesh’s continued progress in the fight to eliminate malaria and improve public wellness especially among those who bear the greatest burden of poor health.
Kasturi Haldar, Ph.D. Editor-in-Chief, PLOS Pathogens, is the Julius Nieuwland Chair of Biological Sciences and Parsons-Quinn Director of the Boler-Parseghian Center for Rare and Neglected Diseases, University of Notre Dame.
Bernard L. Nahlen, M.D. is Professor of Biological Sciences and Director of the University of Notre Dame Eck Institute for Global Health.
Neil Lobo is Research Professor of Biological Sciences, University of Notre Dame Eck Institute for Global Health,
Mohammed Shafiul Alam, Ph.D. is Associate Scientist, Emerging Infections & Parasitology Laboratory, Infectious Diseases Division, icddr, b, Dhaka, Bangladesh.
Wasif Ali Khan MBBS, MHS is Scientist, Infectious Diseases Division, icddr, b; Dhaka, Bangladesh.
Image Credit: Dr. Wasif Ali Khan, icddr,b.
